The COVID-19 coronavirus pandemic may seem unprecedented, but outbreaks of infectious diseases are nothing new.
While there aren't many people who remember what it was like to live through the last intense pandemic — the “Spanish flu” of 1918 — or even the polio epidemics of the 20th century, health crises that took place over the past 100 years are now being used as a sort of roadmap when it comes to addressing COVID-19.
In many ways, countries have never been better equipped to address infectious disease outbreaks as they are today. The efforts of health care workers, government officials, and the public to contain past health crises have greatly informed and shaped the response to the new coronavirus, while the failures of past crises loom over the COVID-19 pandemic, acting as a continual warning and reminder for the urgent need to develop tests, treatments, and vaccines that are equitably distributed around the world.
Here are nine key advances, developed by the medical and scientific communities as a result of past health crises, that the global COVID-19 response continues to incorporate.
Social Distancing
 St. Louis Red Cross Motor Corps are photographed on duty in Oct 1918, during the influenza epidemic.
St. Louis Red Cross Motor Corps are photographed on duty in Oct 1918, during the influenza epidemic.
St. Louis Red Cross Motor Corps are photographed on duty in Oct 1918, during the influenza epidemic.
In 2007, researchers took a close look at how cities in the United States responded to the Spanish flu pandemic in 1918. Philadelphia, Pennsylvania, which ignored early warnings of the virus and held a parade during its approach, ended up having a severe outbreak. St. Louis, Missouri, meanwhile, ordered people to stay indoors and managed to overcome the virus swiftly.
“They found a pretty strong signal that cities that socially distanced early did better than those that did not,” David S. Jones, professor of epidemiology at Harvard University, told Global Citizen. “And then that got built into US policy on how to respond to flu pandemics, and people jumped on that back in February. Whenever people talk about flattening the curve, that’s from a historical analysis of 1918.”
While social distancing may seem like a mundane tactic, its adoption by governments around the world has been a major public health breakthrough.
In the beginning of 2020, social distancing became the first line of defense against coronavirus, and countries that encouraged citizens to stay home early on invariably fared better than those that didn’t.
Community Engagement
Overcoming public health crises depends on the support and protection of all members of a community; otherwise, new outbreaks can occur repeatedly, according to the World Health Organization (WHO).
Throughout the history of pandemics — from the bubonic plague in the 1300s to the SARS outbreak in 2003 — governments have struggled with this rule.
During the West African Ebola crisis of 2014-2016, local governments ran into difficulties when trying to enforce lockdown measures in areas where government suspicion ran high; people lacked access to water and sanitation; and communities relied on wages earned by daily labor, according to Adia Benton, a cultural and medical anthropologist at Northwestern University.
“What do you have to do to make sure people stay at home, and they have no reason to go out? That they’re not losing income, that they're able to eat, they’re able to care for themselves during a lockdown?” she told Global Citizen. “These were considerations that were not taken seriously, to the extent that governments weren’t especially good at giving people the resources they needed.”
Lockdown measures can only work, Benton explained, when governments are transparent about what they’re doing, while also providing robust social safety nets throughout a social distancing period and engaging with community members.
 Karungi Shamillah is a Red Cross volunteer in her community in Majada, Uganda in 2018. Shamillah is trained to conduct community-based surveillance, educate communities about Ebola, while also recognizing the signs of the virus to ensure follow up care.
Karungi Shamillah is a Red Cross volunteer in her community in Majada, Uganda in 2018. Shamillah is trained to conduct community-based surveillance, educate communities about Ebola, while also recognizing the signs of the virus to ensure follow up care.
Karungi Shamillah is a Red Cross volunteer in her community in Majada, Uganda in 2018. Shamillah is trained to conduct community-based surveillance, educate communities about Ebola, while also recognizing the signs of the virus to ensure follow up care.
The WHO notes that the Democratic Republic of the Congo (DRC) incorporated more thorough community engagement into its public health system following the Ebola crisis in 2014-2016, which tailored responses to each affected community when they were faced with outbreaks in 2018 and 2020.
Crowdsourced Science
Throughout the COVID-19 pandemic, amateur scientists have stepped up to 3D-print face shields, develop faster tests, and provide research assistance to major labs.
This sort of community activism has its roots in the HIV epidemic of the 1980s, when LGBTQ+ activists worked on treatment options for the disease and campaigned for government support.
 Protesters, organized by the gay rights activist group ACT UP, lie on the street in front of the New York Stock Exchange on Sept. 14, 1989, in a demonstration against the high cost of the AIDS treatment drug AZT.
Protesters, organized by the gay rights activist group ACT UP, lie on the street in front of the New York Stock Exchange on Sept. 14, 1989, in a demonstration against the high cost of the AIDS treatment drug AZT.
Protesters, organized by the gay rights activist group ACT UP, lie on the street in front of the New York Stock Exchange on Sept. 14, 1989, in a demonstration against the high cost of the AIDS treatment drug AZT.
“HIV activists pushed a people’s science that sped up some of these regulatory processes and showed how you can develop a scientific project of urgency,” Benton said. “That’s given us a framework for accelerating research under these conditions of emergency.
“It helped to change how we think about experimentation in a crisis,” she added.
The AIDS Coalition to Unleash Power, known as ACT UP, helped to streamline the process for developing HIV treatments in the US, a systemic change that has helped researchers greenlight COVID-19 treatments more rapidly today.
Vaccines
The world is waiting with bated breath for a COVID-19 vaccine. Whether one will emerge within 12 to 18 months is unclear, but what is clear is that scientists are developing the vaccine at a faster rate than ever before.
That process — from the research phase to mass production to distribution — was improved during past health crises.
Researchers discovered a vaccine to smallpox in 1798, but it took more than a century to reach most of the world, because countries lacked the ability to mass produce, store, and distribute treatments.
“They rounded up a group of orphans, sent that ship around the world, used each kid to maintain a case of smallpox, and they would take whatever kid had active populations [to vaccinate people],” Jones said. “ It was a cumbersome process.”
In the 1950s, scientists rushed to produce polio vaccines to inoculate populations as polio paralyzed hundreds of thousands of people around the world. They ran into manufacturing problems and critical issues surrounding efficacy — but eventually managed to roll out the vaccine globally in the 1960s.
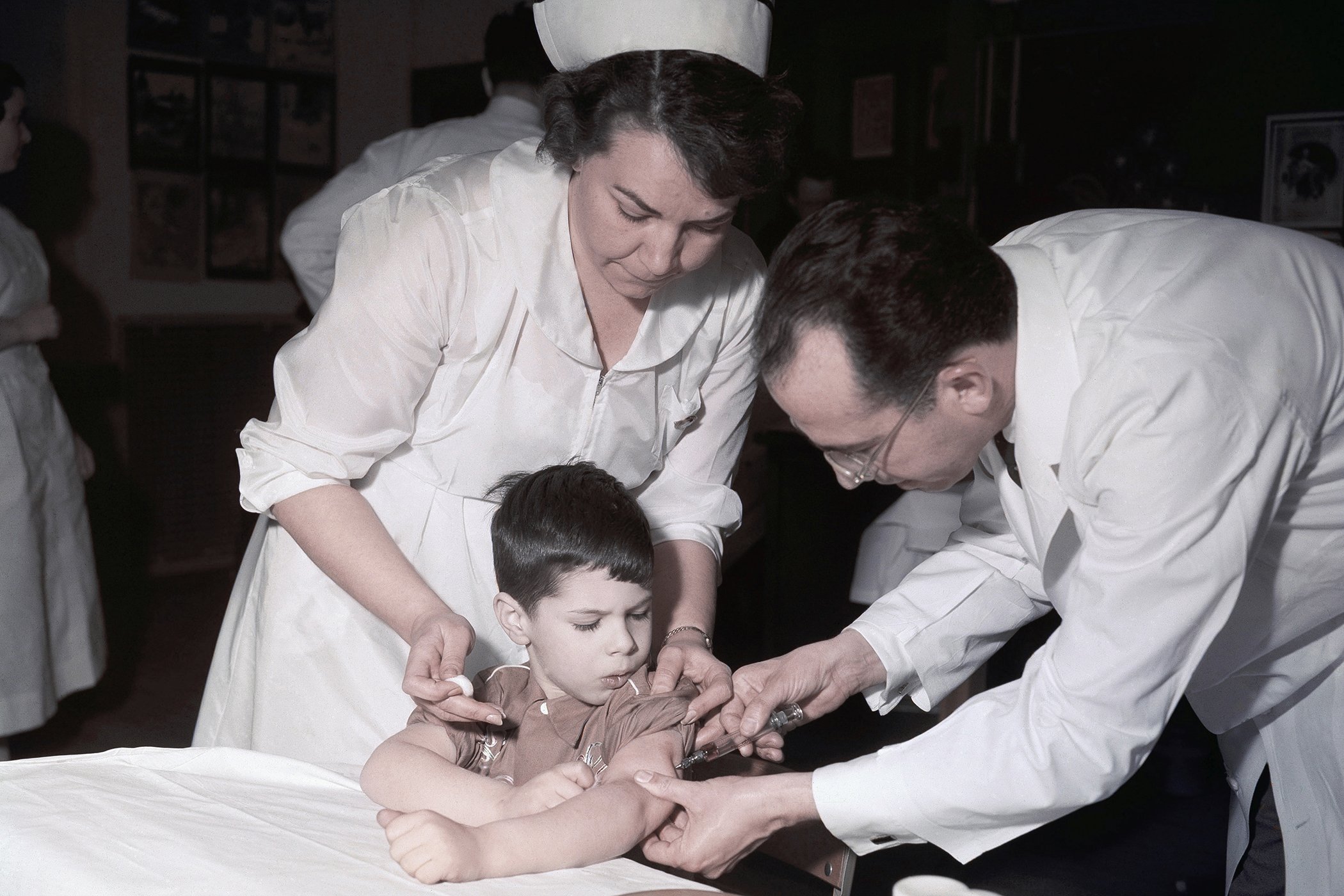 Polio vaccine being administered by Dr. Jonas Salk on April 23, 1964.
Polio vaccine being administered by Dr. Jonas Salk on April 23, 1964.
Polio vaccine being administered by Dr. Jonas Salk on April 23, 1964.
Researchers have learned from past mistakes, new technology has ironed out many of the earlier production complications, and manufacturing capacity has increased exponentially, Jones said.
Still, he suspects that a coronavirus vaccine will run into logistical challenges of its own.
“If you’re going to vaccinate 300 million in the US and 7 billion in the world, you’re going to need a lot of needles and syringes and vials,” Jones said.
Some of the potential challenges, such as vaccine storage and transportation, have been made easier by improvements in technology. Drones can now deliver vaccines to remote areas, and advanced cooling technology can ensure the integrity of vaccines that require refrigeration over long distances.
Other problems, like vaccine aversion and conspiracy theories, can potentially be remedied by pointing to past health crises, Jones said.
Contact Tracing
Many governments waited too long to take proactive measures to contain the current coronavirus outbreak and have faced massive loss of life and severe economic disruption. Others reacted in ways that reduced casualties.
Numerous countries in Southeast Asia reacted quickly to today’s pandemic because of lessons learned from the 2003 SARS crisis. SARS was a deadlier virus than COVID-19, but it wasn’t as infectious, so countries had more time to contain it.
 A health worker measures the temperature of an airline stewardess at the airport in Beijing, China, Tuesday, May 20, 2003.
A health worker measures the temperature of an airline stewardess at the airport in Beijing, China, Tuesday, May 20, 2003.
A health worker measures the temperature of an airline stewardess at the airport in Beijing, China, Tuesday, May 20, 2003.
During the peak of the SARS epidemic, many countries rolled out massive public health campaigns that involved screening people with infrared thermometers (also known as “thermometer guns”), promoting social distancing, and conducting contact tracing.
Contact tracing, which involves tracing anyone an infected person comes into contact with, is a particularly effective tool for preventing outbreaks because it allows health responders to isolate people who could potentially spread a virus. If countries can fully trace a person’s web of contacts, then an outbreak can be stopped more quickly.
“These are countries that were shaken up by SARS in 2003,” Jones said. “Places like Vietnam have totally robust health systems in place [now] to detect early cases of respiratory disease, to do contact tracing, to do all these things.
“They kicked into high gear [for COVID-19], and have had 300 cases with zero deaths, and they share a gargantuan land border with China,” he added.
Countries that contended with Ebola in 2014-2016, such as Sierra Leone, Liberia, and the Democratic Republic of Congo, developed strong systems for screening and tracking people across and within borders. Those protocols have now been redeployed in the fight against COVID-19.
“Countries were pushed to take on the global health security agenda, which isn’t actually about care as [much as] it is about surveillance and the constant vigilant tracking of certain disease threats,” Benton said. “That kind of stuff focuses on technology.”
Contact tracing is not a silver bullet for fighting infectious disease outbreaks, according to the MIT Technology Review. In the case of diseases like COVID-19, which can be passed asymptomatically from person to person, contact tracing only works if testing is widespread and accessible.
In early 2020, South Korean officials rapidly mobilized health workers and resources to test as many people as possible in the early stages of the COVID-19 outbreak. As a result, they were able to effectively trace the contacts of infected citizens.
In the US, on the other hand, a lack of testing has undermined the usefulness of contact tracing, the MIT Technology Review reports. The US currently has the highest number of COVID-19 cases reported in the world.
Data Collection
If countries lack reliable and steady data on hospital visits, treatment methods, risk factors throughout a population, and countless other variables, then containing a viral outbreak becomes much harder.
Carolyn Pullen, chief executive officer of the Canadian Cardiovascular Society, said that the SARS outbreak of 2003 highlighted the urgent need for investments in data collection and data sharing in Canada.
Data collection technology has improved dramatically in recent years, aided in part by artificial intelligence, and organizations such as the WHO have invested heavily in data capabilities.
The advancement of AI has also helped public health officials to better predict outbreaks and determine strategies for addressing them.
However, major gaps persist around the world, Pullen said.
“Real-time data was lacking then and it’s lacking now, so it has hampered our ability to plan resource allocation and map out the trajectory and the hot spots [of the virus] and where to concentrate resources,” she told Global Citizen. “Instead of taking a targeted approach, we’ve had to take a blanket approach and shut down everything.
“If we had better data, we might have been more strategic, but also more effective in how we managed the spread of the [COVID-19] infection,” she continued. “There’s no question that data collection and reporting is expensive and complicated, but we already have the infrastructure in place to do it. We just underfund it.”
Diagnostics
The US response to COVID-19, in particular, has been hampered by both a lack of tests and widespread testing failures.
“COVID-19 has exposed not so much the liabilities of hospitals, but the complete disarray of the US public health system,” Jones said. “We still don’t have adequate testing capacity.”
He said that if the US had applied lessons from past health crises, then testing capacity wouldn’t have been an issue this time around.
Past public health crises have shown how crucial it is to have early and effective diagnostic capacity.
Substantial improvements in technology have made it possible to develop and deploy tests rapidly, according to STAT News. It took scientists more than a year to sequence the genome of SARS, while COVID-19 was sequenced in less than a month. This compressed timeline allowed scientists to create diagnostic tests much faster, and get them into the hands of health workers earlier on.
Scientists have also learned a range of new techniques for devising treatments from past pandemics, the New Yorker reports. The HIV epidemic showed how it can be useful to pursue a multi-drug solution, while the Ebola crisis has benefited from gene-editing technology.
Medical Gear and Hygiene

Much of the medical gear that health care workers rely on to treat COVID-19 patients was developed or improved during past health crises.
The N95 mask and the hazmat suit both have their origins in the Great Manchurian Plague of 1910 in parts of China and Russia, after doctors deduced that the virus was airborne.
During the 2014-2016 Ebola crisis, health care workers relied on advances in smartphone technology to read temperatures, track symptoms, and learn new care protocols. These more accessible forms of health care allowed countries to better contain the virus in areas with few resources.
Methods of hygiene — from disinfecting and ventilating rooms to sanitizing tools to properly disposing of waste — were adopted on a large scale to stop outbreaks of tuberculosis, cholera, and typhoid.
“Hospital treatment has improved immensely over the past century, notably with the availability of antibiotics and vaccines that were unavailable during the last major global pandemic of influenza in 1918,” John Tang, economic historian at Melbourne University, told Global Citizen. "Improved diagnosis and a lower probability of infection, from other patients or unsanitary practices, mean people are less likely to die now in hospitals than historically.”
Pop-Up Hospitals
All around the world, hospitals have been overwhelmed by the surge of COVID-19 patients needing critical care.
Patients have been put in different hospital units, hallways, and lobbies. In many cases, pop-up hospitals were rapidly built to handle the overflow.
Pop-up or tent hospitals were used more than a century ago, during the Spanish flu pandemic to deal with excess capacity, but there were enormous problems with these earlier iterations.
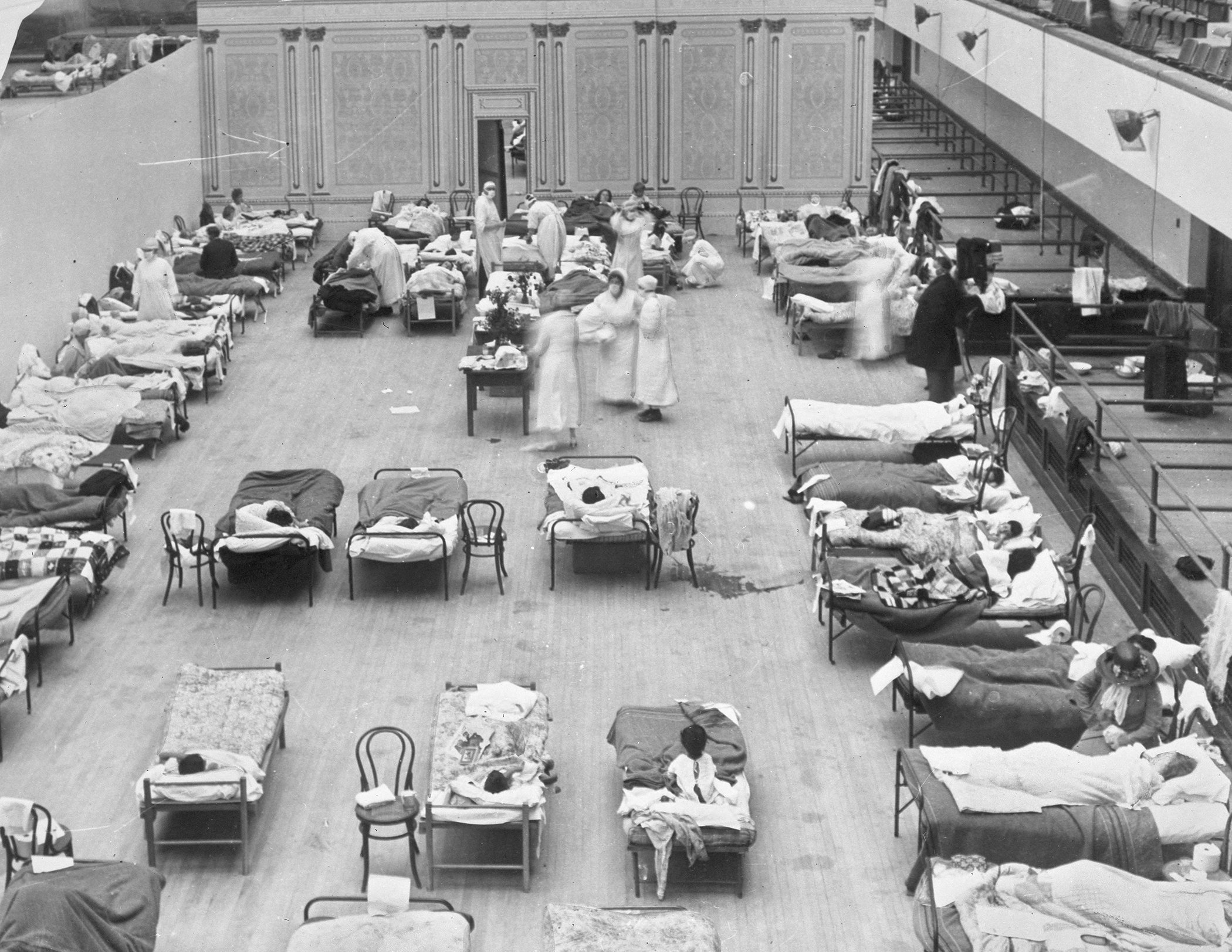 In this 1918 file photo made available by the Library of Congress, volunteer nurses from the American Red Cross tend to influenza patients in the Oakland Municipal Auditorium, used as a temporary hospital.
In this 1918 file photo made available by the Library of Congress, volunteer nurses from the American Red Cross tend to influenza patients in the Oakland Municipal Auditorium, used as a temporary hospital.
In this 1918 file photo made available by the Library of Congress, volunteer nurses from the American Red Cross tend to influenza patients in the Oakland Municipal Auditorium, used as a temporary hospital.
“In 1918, you could provide all the medical care in a tent as you could in a hospital, but there was no ventilator, no oxygen support, no IVs; all you could provide was moral support, food, and hygiene,” Jones said.
Since then, major technological advances have made pop-up hospitals a more viable option as access to resources has improved, as well as the ability to provide treatments in a pop-up setting.
In New York, for instance, the Jacob Javits Convention Center was converted into a state-of-the-art hospital within days.
While past lessons have greatly helped some countries respond to today’s pandemic, progress remains uneven between and within countries — and public health investments often get delayed or neglected.
“There are many lessons from past health crises that are still being ignored, namely a vigorous response, coordination, and preventative measures,” Tang said.
“It is also irresponsible to treat health care like a competitive industry, cutting back slack to save on short run costs. Epidemics are rare, but they can easily overwhelm the number of hospital beds and medical staff operating at normal capacity,” he added. “Does this generate inefficiency? Perhaps, but the alternative is unnecessary deaths and economic pain. These consequences are also not randomly distributed, but disproportionately affect the vulnerable and marginalized.”
Jones said that he hopes the failures in response to COVID-19 spur countries to invest in public health. More robust surveillance and contact tracing measures would have contained the pandemic sooner, he said. And if countries had actually stocked up on essential supplies, then there wouldn’t have been personal protective equipment shortages.
Benton said that it’s unclear what the legacy of COVID-19 will be — will countries invest in health care systems and social safety nets? And will the long-term care and well-being of communities be prioritized?
Pullen was more confident that the pandemic will lead to lasting change.
“Everyone right down to the youngest toddler is going to remember what this was like and how it shut down the world, and the health and economic consequences, it’s so sweeping,” she said. “My hope is that the total population’s awareness of what it means when things go wrong strengthens the political will this time.”
She added: “I really believe people will say, ‘Let’s do everything we can to not have anything this catastrophic unfold again.’”