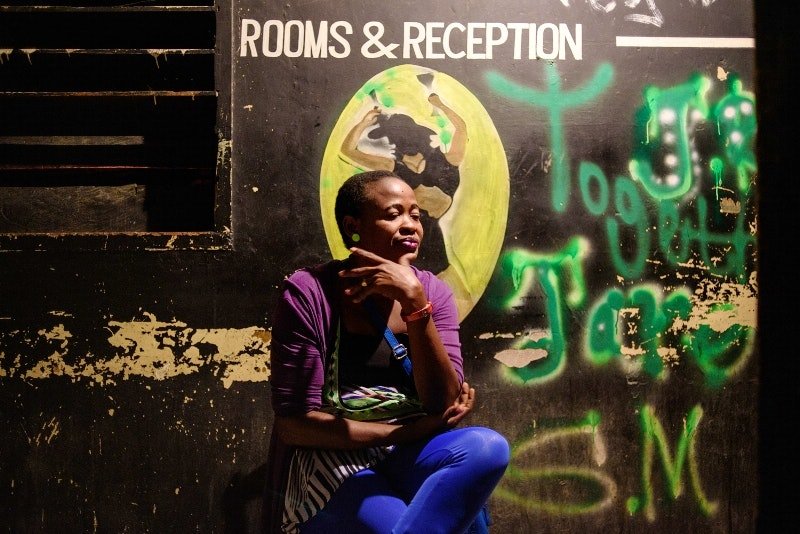HOMA BAY, KENYA – Shantel sits in a bar lit by TV screens. Wet bottles of Tusker beer line the shelves, low cushioned chairs crowd the floor. A client waits for her in a back room.
Shantel’s parents died when she was 15, leaving her and her sister Magdari alone. “My parents died with HIV so I didn’t have anywhere to go. It’s when I started sex work,” she says. “I was desperate. I just decided to come [to Homa Bay town] and look for money. It was difficult because I was still young. When I went to clubs, I was being beaten. [People were saying:] ‘This small child, what is she coming to do here?’ So it was hostile, it was not easy for me.”
Homa Bay County, on the shores of Lake Victoria in western Kenya, has an HIV prevalence rate of 26 percent, the highest in the country. Thousands of children have lost their parents to AIDS-related illnesses. The area’s economy runs on its fishing industry, and young girls like Shantel who are orphaned have few options but to go to the shores of Lake Victoria every morning to exchange sex for food or money.
Read More: Meet Grace Wairimu, the Girl Who Sings For a Future Free of HIV
“I was getting a little that could sustain me,” says Shantel, now 18. She started by offering men “shots” – quick sex for 500 shillings ($4). “But it was difficult. If he wants [sex] freely without condoms, you’ll be beaten up, and you know there’s nowhere you can go and report it.”
Until recently, police in Homa Bay were indifferent or hostile to sex workers, but a 2015 program supported by the Elizabeth Glaser Pediatric AIDS Foundation (EGPAF) helped change their stance.
“We did a sensitization program with the police,” says Eunice Ojollah, a social worker at Makongeni Health Center, the only health facility in the area that offers free treatment and counseling for sex workers and their children. “We told them that we need to protect these people … They have their rights as sex workers, they have their rights as women, as our mothers, our sisters. So [the police] understood us and they have been helping on violence cases.”
There is no data yet on the young program’s impact, but anecdotally, authorities say they have seen a reduction in violence against sex workers since it began. If a client gets violent, now sex workers know they can go to the police.
Read More: How a Sex Worker Led This Doctor to Groundbreaking HIV Discovery
With the area’s HIV rates rising over the past decade, EGPAF also initiated the “key population” program in 2015, to enlist sex workers like Shantel to be peer educators, and hand out condoms to other sex workers in the bars and beaches around Homa Bay.
Evaline is one of the 489 sex workers currently involved in the program. “As peer educators, we talk to girls about using condoms,” she says. “We tell them they should not go into a room with a man if they are drunk. If the man is drunk, tell peers. It’s you who must put the condom on the man directly. We have female condoms, too.”
Sex educators such as Evaline remain in contact with the women and girls they advise, often visiting them at home and making sure they get regular health checkups.
“Those who are HIV-negative, we need to test them [for HIV] after every quarter,” says Ojollah, the social worker at Makongeni Health Center. “For those who are HIV-positive, we need to see them after three months for [sexually transmitted infection] screening and maybe family planning and follow-up on the viral loads. It helps us to follow up on their progress of HIV care.” The center also offers HIV-positive women anti-retroviral drugs for free.
Read More: The Dangerous Conditions Facing Newborn Babies of Sex Workers
Ojollah says that in the two years since the key population program started, there has been only one seroconversion – when the body develops HIV antibodies – among the women who were HIV-negative. “We are happy with that because it means they are using condoms consistently, they are adhering to what we are teaching them,” she says.
And over time, the stigma against sex workers has also reduced, she says.
“[The community] has accepted that they are here to stay. They are somebody’s sister, somebody’s mother. If we leave them out, we won’t succeed in fighting HIV/AIDS.”