As the COVID-19 coronavirus spreads throughout the US, long-standing inequalities in the country’s health care system are being exposed and many people are dying as a result.
One woman in Pennysylvania died after refusing to go to the hospital because she feared that it would cost too much, while a man died after "self-medicating" with a chemical found in a fish tank cleaner because of misinformation. Another man used his last breath to ask the doctor "who’s going to pay for" the cost of a life-saving ventilator.
People of color, especially black people, are dying at a higher rate in the US from the coronavirus than white people because they’re more likely to work in jobs that can’t be done remotely, have less access to health insurance, and have pre-existing conditions related to poverty, according to researchers who spoke with the New York Times.
Black people in the US are also more likely to live in areas with severe air pollution, which increases the likelihood of dying from the virus.
The COVID-19 coronavirus isn’t the first health crisis to highlight inequalities in US health care. Across the country, people of color and people living in poverty have less access to quality health care and face a range of health consequences not experienced by other Americans.
In some parts of the US, even Neglected Tropical Diseases (NTDs), which generally affect people living in extreme poverty, flourish.
Now, as the COVID-19 pandemic threatens to kill hundreds of thousands of people living in the US, the country’s historic failure to guarantee health care and provide basic human rights, like quality water and sanitation, raises significant questions about its ability to effectively protect people against coronavirus.
Diseases of Poverty
NTDs including toxocariasis, trichomoniasis, neurocysticercosis, and Chagas disease infect tens of millions of Americans. Due to a lack of awareness surrounding these diseases, and widespread lack of health care coverage, many of the people impacted by them are unaware.
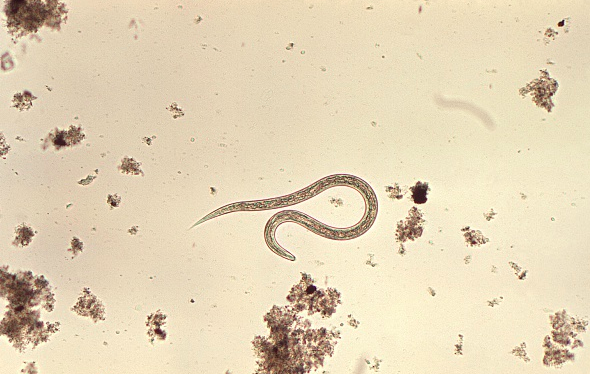
A few years ago, researchers at Baylor University traveled to Lowndes County, Alabama, to study the prevalence of hookworm, an NTD that causes anemia, gastrointestinal issues, and chronic fatigue, and disrupts the development of children.
Long thought to be eradicated in the US, no major study had been done on the parasite in the country since the 1950s, Rojelia Mejia, a physician who helped lead the Baylor University study, told Global Citizen.
His team’s research ultimately shows the ways in which certain populations in the US are denied basic human rights like health care, a clean environment, safe water, and adequate sanitation. This multi-dimensional poverty, in turn, leaves communities exposed to a range of preventable diseases, Mejia said.
In Lowndes County, where 74% of residents are black and the average annual income is less than $20,000, nearly 3 in 4 people lack adequate sanitation systems and are exposed to raw sewage on a regular basis. Some people report having raw sewage flood their homes during rainstorms; while others have dried water lines flecked with feces along the walls of their homes.
Hookworm at Home
Hookworm is a distant threat in places with functioning sewer systems. But in areas with poor sanitation systems, or where people practice open defecation, human waste regularly washes into water supplies, farmland, and even into people’s homes.
People then get hookworm by drinking contaminated water or walking barefoot over areas that have been contaminated by feces.
As a result of the sanitation crisis in Lowndes County, roughly a third of its residents could be infected by hookworm, according the Baylor University study.
The prevalence of hookworm can cause serious health problems for residents and is especially harmful to children.
Children who become infected with hookworm can experience nutrient deficiencies that impede mental and physical development, and undermine academic outcomes.
"You’re basically fighting an organism for nutrition and you already have food scarcity and a poor diet, so if you have a parasite and you have these physical and cognitive delays, then you don’t do as well in school, you don’t finish school, and you have less opportunities [compared to] kids who didn’t have a parasite," Mejia said. "You could almost say it’s a circle. Poverty increases your risk of parasites, then those same parasites impact your children, who are at a greater risk of living in poverty."
Targeted investments and government assistance could end the health crisis, which could ultimately reduce poverty in the region, Mejia said.
Eliminating the disease comes down to modernizing sanitation systems and eliminating exposure to raw sewage, but people affected by the parasite are often unable to afford a new sanitation system, which can cost around $15,000.
Mejia said that his team is exploring ideas for communal sewage tanks that families can share, and potentially adding something to sanitation systems that could kill hookworm eggs.
His mentor, Peter Hotez, is working on a hookworm vaccine — a discovery that could protect the health of up to 740 million people worldwide.
For people who have hookworm in the US, highly effective treatments are available. But many people who have hookworm don’t know they have the infection — and many people who have tested positive for the parasite are often unable to afford the treatment, Mejia said.
Poverty and Health
Hookworm treatment plans in the US cost an average of $400, which is several hundred times more expensive than treatment is elsewhere, according to Mejia. Considering nearly 40% of Americans are unable to afford a $400 emergency, and the average household in Lowndes County lives below the poverty line, the hookworm treatment plan is often too expensive for people who need it.
Even when people do get treatment, they often get infected again when they return home, which highlights the need for structural interventions like improved sanitation systems.
"The eggs last in the environment for months," Mejia said. "So people get continuously reinfected."
Preventing hookworm is a public health matter because it transmits from person to person; once you break that chain, the parasite disappears.
This is where hookworm and coronavirus coincide — at the intersection of poverty, environment, and race, where preventable diseases often ravage communities that have been systematically neglected.
"COVID-19 will have a bigger impact on African Americans, but also Latinos and anyone below the poverty line," Mejia said. "Just like COVID-19, these parasites affect people below the poverty line more."
In rural areas of the South where hookworm flourishes, hospitals and health care facilities are often understaffed, underfunded, and have out-of-date technology, according to the Guardian.
Over the past decade, 128 rural hospitals have closed in the US because of persistent underfunding. Oftentimes, closures happen because states refuse to accept Medicaid funds from the federal government through the Affordable Care Act.
As the coronavirus spreads in rural communities that have poor health care coverage, facilities could become overwhelmed and struggle to provide adequate care to patients. Many people may avoid getting treatment to avoid debt, and for those who do get treatment, they may end up with bills that push them further into poverty.
Already, two-thirds of rural counties in the US have reported coronavirus infections.
In Lowndes County, the number of COVID-19 infections recently surpassed 40. If people aren’t getting tested and treated, and have preexisting conditions like hookworm, then coronavirus could quickly spiral out of control.
How these areas overcome the virus depends in large part on the resources that health care facilities receive and the support given to people infected.
The coronavirus pandemic is a long-overdue wake-up call. Millions of people throughout the US lack access to basic health care and fundamental human rights like basic sanitation that foster good health.
Protecting marginalized groups throughout this crisis requires structural investments that will also protect them from a cascade of other illnesses — including hookworm.