Mirriam Banda Chisamba, a midwife in Zambia, was working every day without access to personal protective equipment (PPE) this past March when the World Health Organization (WHO) declared COVID-19 a pandemic.
“I was fearing for my life. What if I contracted COVID-19? How would I live? What if I died? What would happen to my family, my children?” the mother of three told Global Citizen.
Banda Chisamba, who works at Kafumbwe Rural Health Center in Katete District, had only gloves and a surgical mask for protection during interactions with patients, while her international counterparts were accessing PPE including face shields and respirators that filtered out airborne particles.
The Centers for Disease Control and Prevention (CDC) now knows that COVID-19 spreads through respiratory droplets or small particles “formed when a person who has COVID-19 coughs, sneezes, sings, talks, or breathes.”
But at the time, little was known about coronavirus and how it spread. Banda Chisamba was told to assume it was COVID-19 if she encountered anyone with symptoms like a fever and dry cough.
“That’s all we were working with,” she said.
The uncertainty was nerve-wracking.
The Kafumbwe Rural Health Center is on a main road near the border with Mozambique. Banda Chisamba was terrified that truck drivers who frequently crossed the border would transmit the virus locally, and put further strain on the small, poorly-equipped health clinic.
The center, which serves a population of 12,000, does not employ a doctor and has one clinical officer. Staff often take on additional roles, and Banda Chisamba sometimes screens, diagnoses, and provides treatment to pregnant women and children under 5 — going beyond her primary duties as a midwife.
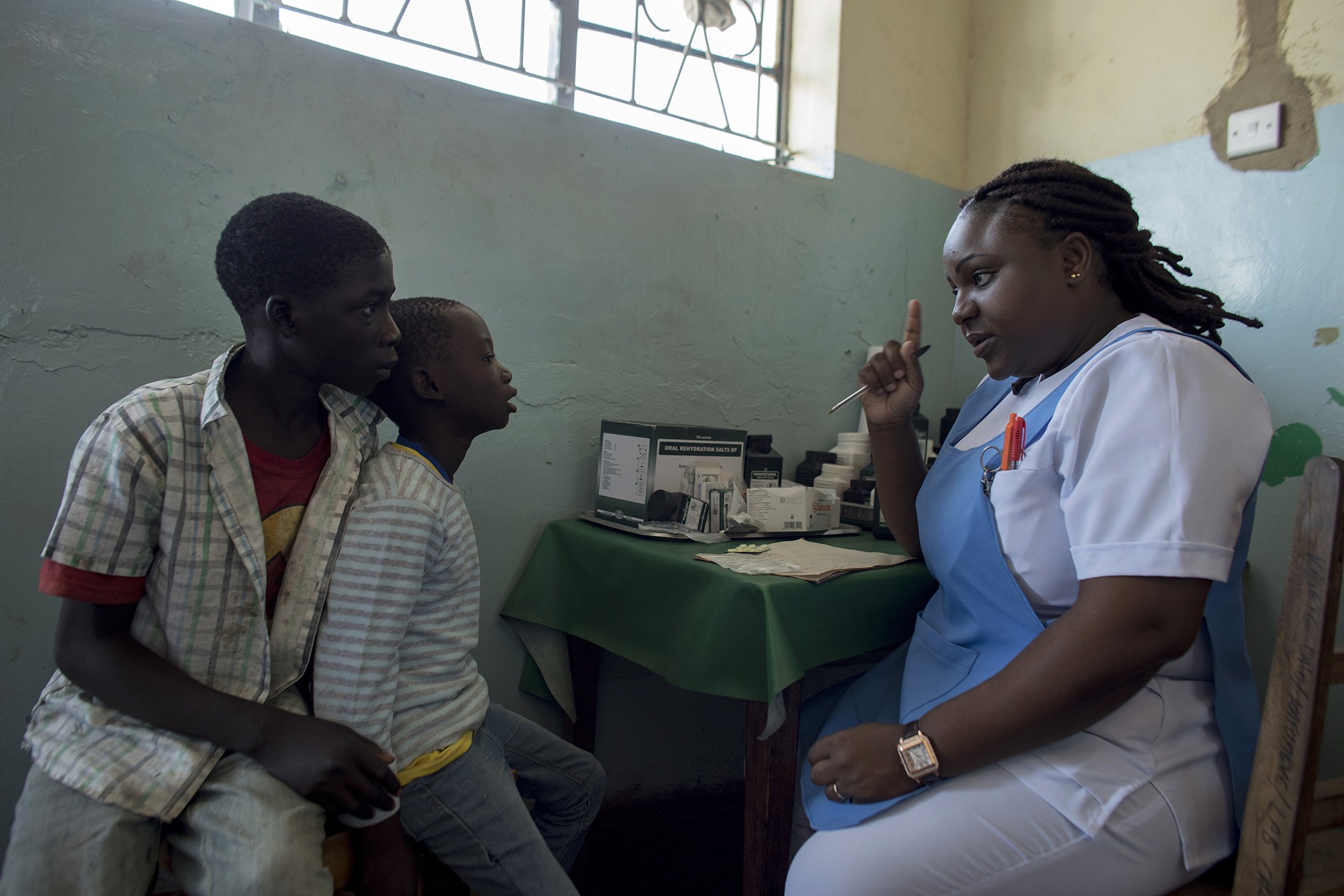 Mirriam Banda Chisamba speaks with patients at Kafumbwe Rural Health Center, Katete District, Eastern Province of Zambia.
Mirriam Banda Chisamba speaks with patients at Kafumbwe Rural Health Center, Katete District, Eastern Province of Zambia.
Mirriam Banda Chisamba speaks with patients at Kafumbwe Rural Health Center, Katete District, Eastern Province of Zambia.
She continued to see pregnant patients, checking their blood pressure, palpating the abdomen, and checking fetal heartbeats.
“Being at a health facility, you have to continue working,” she told Global Citizen. “We were just praying, ‘God, let me not be a victim. I’m here helping others so let me survive.’”
By the end of April, the center had received a shipment of PPE, including hazardous material suits, masks, shields, hand sanitizer, and safety boots. International partners donated the PPE to Zambia, which reached Lusaka, the country’s capital, before being sent by the health ministry to the provinces, districts, and finally, the rural health clinics that needed it — including Banda Chisamba’s.
As of Dec. 7, Zambia had recorded 17,916 cases of COVID-19 and 364 deaths. So far, Banda Chisamba’s health center has not recorded any cases. When Banda Chisamba encounters a patient with symptoms, she notifies the district's main lab. They send health workers to collect swabs. COVID-19 testing, which initially took weeks, has sped up in Zambia. Nowadays, it takes less than a week to get results.
Testing is provided at no cost, like all other services, at the government-run Kafumbwe Rural Health Center. In Zambia, medical care is free or heavily subsidized. The country is piloting a universal health insurance program to make health care more accessible to those most economically disadvantaged.
 The Kafumbwe Rural Health Center is on a main road near the border with Mozambique. The center, which serves a population of 12,000, does not employ a doctor and has one clinical officer.
The Kafumbwe Rural Health Center is on a main road near the border with Mozambique. The center, which serves a population of 12,000, does not employ a doctor and has one clinical officer.
The Kafumbwe Rural Health Center is on a main road near the border with Mozambique. The center, which serves a population of 12,000, does not employ a doctor and has one clinical officer.
Banda Chisamba, an advocate for the Global Fund to Fight AIDS, Tuberculosis, and Malaria since 2017, is vocal about the role of international donors in ending diseases like malaria, TB, and AIDS in Zambia.
She points out that as most local people earn a small income through farming, without donors, the sick would not be able to receive treatment for free. Combating these diseases hits close to home, as her husband is HIV-positive.
“He is living a healthy, normal, productive life because of the antiretroviral drug he is receiving. He doesn't pay anything,” she said.
More than 1 in 10 Zambians has HIV, and nearly 80% receive antiretroviral treatment. The President’s Emergency Plan for AIDS Relief (PEPFAR), a United States government initiative, funds the majority of Zambia’s HIV response. The Global Fund, a partnership of governments, civil society, and communities impacted by disease, has disbursed more than $1.3 billion into tackling malaria, TB, and AIDS in Zambia.
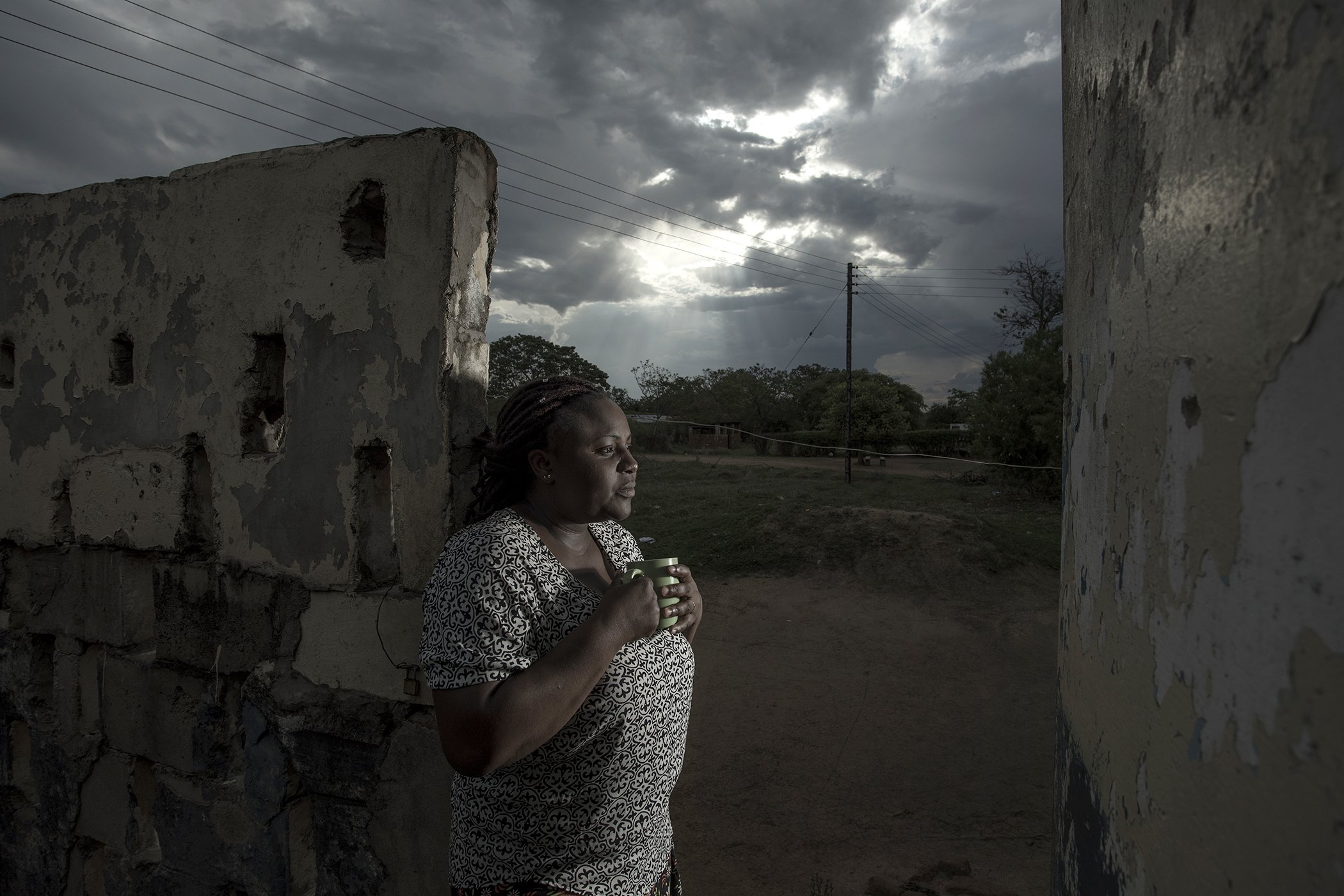 Banda Chisamba, an advocate for the Global Fund to Fight AIDS, TB, and Malaria since 2017, is vocal about the role of international donors in ending diseases like malaria, TB, and AIDS in Zambia.
Banda Chisamba, an advocate for the Global Fund to Fight AIDS, TB, and Malaria since 2017, is vocal about the role of international donors in ending diseases like malaria, TB, and AIDS in Zambia.
Banda Chisamba, an advocate for the Global Fund to Fight AIDS, TB, and Malaria since 2017, is vocal about the role of international donors in ending diseases like malaria, TB, and AIDS in Zambia.
“I believe if we work together, we can raise our voices and fight these diseases,” Banda Chisamba said.
The same is true for COVID-19.
In order to tackle this global health crisis, the international community must band together — which is the driving force behind the Access to COVID-19 Tools (ACT) Accelerator, the global coalition of partners, including the Global Fund, that is working to speed up efforts against COVID-19.
Following the A-Team is a content series that profiles the women working on the ground to combat COVID-19 via the ACT-Accelerator.
Launched in April by seven global partners, the ACT-Accelerator is a unique coalition aimed at accelerating global efforts against the COVID-19 pandemic. Its members are working together to develop tests, treatments, and vaccines as quickly as possible, while also strengthening the world’s most fragile health systems.
The organization desperately needs financial support from governments around the world. You can join us in calling on world leaders to fund the ACT-Accelerator by taking action here.
Disclosure: This series was made possible with funding from the Bill and Melinda Gates Foundation. Each piece was produced with full editorial independence.