Every day, Noluthando Nontobeko Mhlongo wakes up at 4 a.m. and heads to her kitchen to cook for the taxi drivers in her neighborhood. She makes beef, chicken, rice — whatever her customers have requested that day. Phuthu, the traditional South African porridge made from maize flour, is a customer favorite.
But running her home kitchen is only a part-time job for Mhlongo. By 8 a.m., after her early morning cooking shift, the 31-year-old is working as a community health worker. Her work includes tracking down people who have defaulted on their medication or delivering supplies to those who are unable to make it to the clinic. Throughout the four waves of COVID-19 that South Africa has sustained thus far, Mhlongo has also helped out with contact tracing, testing, and combating vaccine hesitancy.
On Mondays, Mhlongo leaves her house in Inanda, a township in the KwaZulu-Natal province of South Africa, to report to the Phoenix Community Health Centre, where she attends weekly team meetings. At the meeting on Nov. 22, 2021, the team leader alerted them of a rise in the country’s COVID-19 cases and warned them of what would become a fourth wave.
“We were so scared because, all the time, when they say there’s a new wave, most of the people will just die,” Mhlongo told Global Citizen. “I’ve seen COVID killing people. I know COVID is real. So I’m always scared — scared for myself, for my family, for my colleagues.”
 Noluthando Mhlongo prepares food that she will eat during her lunch break at Phoenix Community Health Centre in Phoenix, north of Durban on March 14, 2022.
Noluthando Mhlongo prepares food that she will eat during her lunch break at Phoenix Community Health Centre in Phoenix, north of Durban on March 14, 2022.
Within days of Mhlongo’s team meeting, South Africa saw its COVID-19 cases jump exponentially. This worrisome trend led the country’s scientists to identify the presence of a new variant, which the World Health Organization (WHO) named Omicron and declared a variant of concern.
In the months that followed, the highly-infectious Omicron variant forced countries around the world to cancel flights, shut down businesses, and revert to lockdowns. It drove global COVID-19 cases above 1 million per day for the first time during the pandemic, a number that grew to more than 3 million per day in January of this year.
Cases have been on the decline again since then, but these waves will likely continue. As new subvariants surface, one thing is clear: The inequitable access to vaccines on the global scale has allowed COVID-19 to spread, mutate, and threaten both international public health and the global economy. Vaccine inequity is keeping the virus alive.
For health care workers like Mhlongo, another wave could mean yet another period of toiling in an overcrowded clinic and seeing dead bodies every day.
When Self-Interest Becomes Self-Sabotage
More than a year after COVID-19 vaccines have become available, it is apparent that early vows to prioritize equitable access on a global scale have not translated into action. Instead, the global vaccination campaign against COVID-19 succumbed to the influence of wealth and the desire to profit. As countries rushed to secure doses for their own populations, the intent to ensure vaccine equity fell by the wayside.
The result is a severe global imbalance in the distribution of COVID-19 vaccinations. In high-income countries, 74% of people are fully vaccinated (with two doses or equivalent), compared to only 12% in low-income countries. Regionally, Africa has fallen significantly behind. Only 16% of the region’s population are fully vaccinated. In stark contrast, the US, Canada, and Europe have already administered booster shots to an average of 40% of their populations.
The lack of vaccination coverage in low- and middle-income countries has given the virus more of a chance to mutate and potentially evolve into variants that are more infectious, dangerous, or capable of evading current vaccines. The Omicron variant demonstrates the ongoing threat to public health and economic stability we face as a result of global vaccine inequity.
It’s the self-interest of countries in the Global North that enabled the pandemic to spiral into what it is today, said Rosemary Flowers-Wanjie, a policy analyst at the consultancy firm Development Reimagined. By sticking to a “me-first” approach, rich nations disregarded an essential characteristic of the virus — it does not respect borders. As long as it exists anywhere in the world, COVID-19 will continue to be a threat to the international community.
“Global North countries should be participating in the distribution of vaccines in an equitable way not only because that’s a good thing to do, but because it actually benefits them in the long run,” Flowers-Wanjie told Global Citizen. “If we had actually done it from the beginning in an equitable way, we would not be in this position now where we are seeing, every few months, every season, a new variant that concerns us.”
Even before COVID-19 vaccines went into production, rich countries were striking deals with vaccine manufacturers and pre-ordering enough doses to cover their populations several times over. Meanwhile, low- and middle-income countries struggled to secure enough doses to protect even their most vulnerable populations, such as the elderly and health care workers.
Along the same vein, when Omicron emerged, countries in the Global North scrambled to impose travel bans — a rather futile measure at that point — and authorize booster shots for their own populations. Some might argue this form of self-preservation was right in the moment, but it was not a sustainable solution towards ending the pandemic.
“The issue is that this is actually a worldwide problem and this will come back to Global North countries,” Flowers-Wanjie said. “As long as COVID-19 is able to be transmitted through populations, and the longer we have that happen, the more likely it is that we will have variants develop, and the more likely it is that we will eventually have a variant that is resistant to our vaccines.”
A Global Initiative That Lacked Solidarity
 A UNICEF worker checks boxes of the Moderna vaccine after their arrival at the airport in Nairobi, Kenya on Aug. 23, 2021.
A UNICEF worker checks boxes of the Moderna vaccine after their arrival at the airport in Nairobi, Kenya on Aug. 23, 2021.
The global imbalance in COVID-19 vaccination exists despite mechanisms in place that aimed to ensure equitable and fair access. The main mechanism is COVAX — a joint venture between the WHO, the Center for Epidemic Preparedness and Innovation (CEPI), Gavi, the Vaccine Alliance, and UNICEF.
The idea was that COVAX would gather funding from participating countries, as well as public and private organizations, to pre-purchase huge quantities of vaccines. Once these vaccines were made available, the program would then distribute the doses to participating countries equitably, based on the size of their populations.
This strategy would allow smaller nations to access vaccine doses at the same price as larger countries, rather than forcing them into a bidding competition. It would also provide funding for 92 of the world’s poorest nations to get vaccines for free. The ultimate goal was to ensure that the most at-risk groups in each country were protected from the virus as soon as possible.
Unfortunately, what actually happened was a process tainted by supply chain issues and vaccine hoarding. Although virtually all countries signed on to COVAX, rich nations ended up striking separate deals with vaccine manufacturers as well. The prioritization of these bilateral deals limited COVAX’s ability to procure vaccines in a timely manner.
Candice Sehoma, advocacy coordinator for the Access Campaign at Médecins Sans Frontières (MSF, or Doctors Without Borders), calls wealthy nations’ actions “another no-show of global solidarity.”
“It’s nothing new,” Sehoma told Global Citizen. “It’s basically a repeat of how we do things, how the global system has functioned. It functions in a way that puts low- and middle-income countries, countries in Africa, at a disadvantage.”
According to Development Reimagined’s August 2021 analysis, Africa could have had enough vaccines to cover 52% of its population if its countries had actually received all of their orders up to that point. Instead, only 4.5% of the continent’s population had been vaccinated at the time. As of the month of April, the number of people at least partially vaccinated in Africa accounts for 21% of the population.
For Mhlongo, working in KwaZulu-Natal, the delay in vaccinations in her country meant that she has had little time to rest and feel safe. She recalls the overwhelming experience of working at the clinic during South Africa’s third wave of COVID-19. The hospital nearby was so overwhelmed that the 25-bed clinic where she worked was forced to create an isolation unit to accommodate the hospital’s unattended patients.
“It was always full and people were always dying,” Mhlongo said. “It was very rare for a person to die at the clinic [before], but with COVID, you would pass by and see eight bodies a day, 10 bodies a day.”
At the time, only about 1% of Africa’s population had been fully vaccinated. The Delta variant — which drove South Africa’s third wave — led to the continent’s deadliest stage of the pandemic, causing a 43% week-on-week rise in COVID-19 deaths in July 2021 as hospitals filled up and oxygen supplies were stretched thin.
Mhlongo herself was diagnosed with COVID-19 back in July 2020, and her mother, brother, and family friends would go on to contract the virus in the months following. One of Mhlongo’s colleagues, another community health worker at the clinic, died of COVID-19 before the vaccine became available.
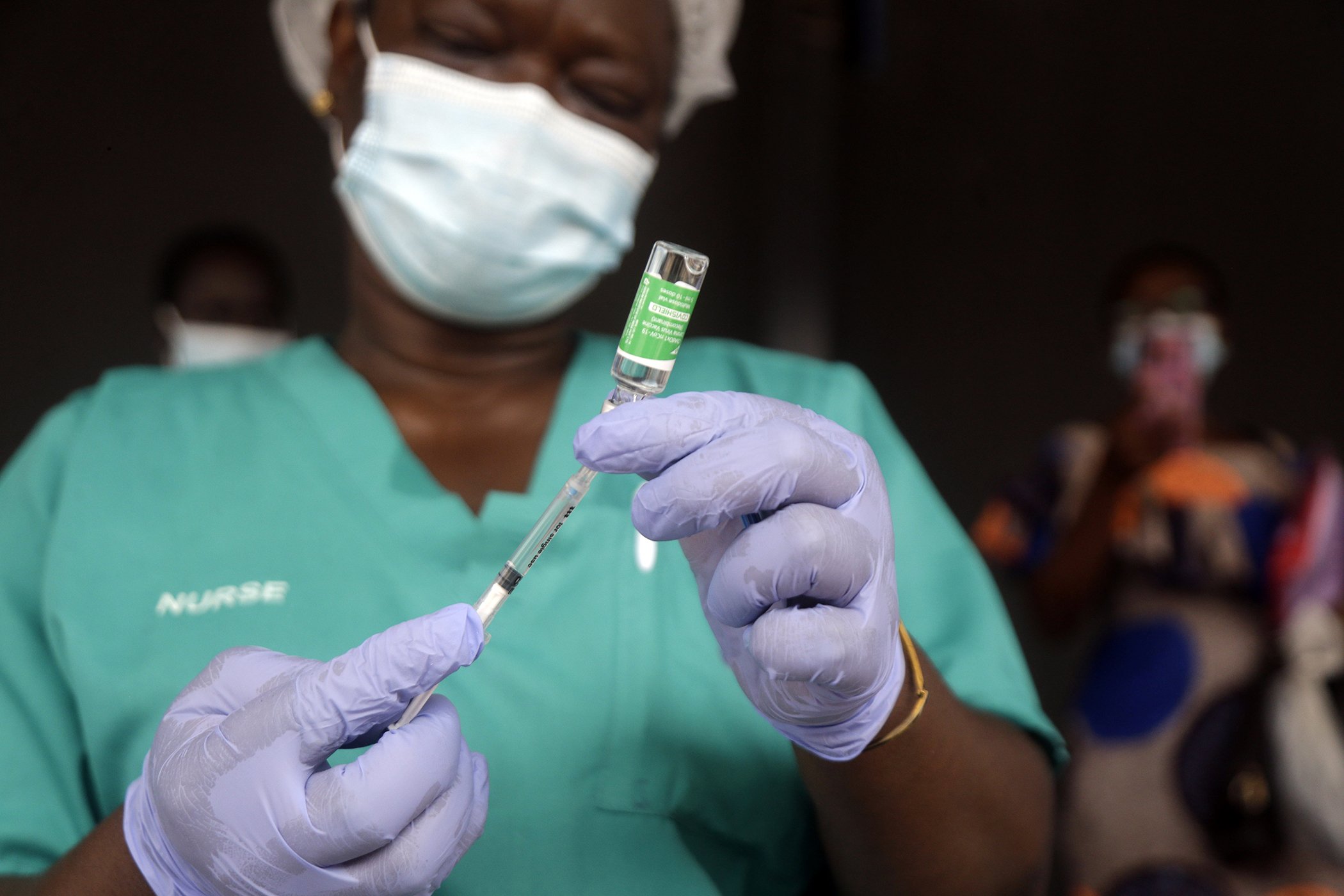 A nurse prepares one of the country's first COVID-19 vaccinations, provided through the global COVAX initiative, at Mainland Hospital Yaba in Lagos, Nigeria on March 12, 2021.
A nurse prepares one of the country's first COVID-19 vaccinations, provided through the global COVAX initiative, at Mainland Hospital Yaba in Lagos, Nigeria on March 12, 2021.
At this moment, the main challenge when it comes to vaccines is no longer on the supply side. By the end of 2021, the demand for vaccines in Global North countries had decreased and global supply chain issues had largely been resolved. This allowed COVAX to speed up its vaccine distribution efforts dramatically. As of April, the initiative has delivered more than 1.4 billion doses to 145 countries and territories.
But barriers remain in the effort to deliver vaccines to the communities that need them most. Weak health systems and infrastructure in lower-income countries make it particularly difficult to transport COVID-19 vaccines — which require cold chain equipment — from the country’s airport all the way to the towns and villages where the doses are administered. Delivery issues have forced the Africa CDC to ask for more staggering in vaccine donations so that doses can be administered before they expire and not go to waste.
Other challenges include a lack of trained health workers and the logistics and data management that go into mass vaccination efforts. Combating vaccine hesitancy and mobilizing the community have also become priorities.
Initiatives have been underway to help fix these issues. Global VAX, for instance, is a US effort put into place to scale up vaccination support in sub-Saharan Africa by bolstering cold chain supply and logistics, service delivery, vaccine confidence, and more. COVAX is also expanding its responsibility beyond vaccine supply to focus on delivery support to countries that are furthest behind.
These initiatives and many more have been crucial to tackling this new phase of challenges. But it will take a conglomerate of actors at the international, national, and local levels, as well as more funding to ensure that all countries reach the global target of fully vaccinating at least 70% of their populations this year.
The Barriers Created by Politics and Profit
There’s little doubt that health inequity and injustice have prolonged the pandemic for everyone. Looking forward, as new variants emerge, ensuring a sufficient supply of tests, vaccines, and treatments will be key to keeping the virus under control and people around the world protected.
That is why more than 100 countries continue to support the Trade-Related Aspects of Intellectual Property Rights (TRIPS) waiver, a pathway to unlock certain intellectual property (IP) rights to allow producers around the world to make and maximize access to COVID-19 medical tools.
In 1995, the World Trade Organization (WTO) introduced TRIPS, a series of global agreements around IP and how to protect it. For pharmaceutical inventions like the COVID-19 vaccines and treatments, TRIPS provides a company with the exclusive right to sell its product and charge whatever price it wishes.
During a public health emergency like the pandemic, these IP restrictions limit the production of life-saving resources that could also be manufactured in low- and middle-income countries. The companies that own these vaccines, however, reap the benefits from the market economy. In November 2021, Pfizer-BioNTech and Moderna were making combined profits of $65,000 a minute, or $93.5 million a day.
“Pharmaceutical companies basically get away with profiteering from people’s lives because they are protected by the IP system,” Sehoma said.
 Scientists conduct research at an Afrigen Biologics and Vaccines lab in Cape Town, South Africa on Oct. 19, 2021.
Scientists conduct research at an Afrigen Biologics and Vaccines lab in Cape Town, South Africa on Oct. 19, 2021.
Anticipating these barriers, a group of countries, led by India and South Africa, proposed the TRIPS waiver in October 2020. The idea was to temporarily waive IP rights, including patents, trade secrets, know-how, and undisclosed clinical data, on vaccines and other medical tools to allow more countries to produce their own supplies, rather than wait for the charity of richer nations.
As was the case for COVID-19 vaccines in 2021, COVID-19 treatments like Pfizer’s Paxlovid are not available in lower-income countries because rich countries get priority access, while Big Pharma monopolizes the initial market. If more effective variant-specific mRNA vaccines become available, IP restrictions would create the same problems while the virus continues to evolve.
“History has taught us that we cannot rely on pharmaceutical companies,” Sehoma said. “We’ve seen this with TB, HIV, and cancer. That’s why it’s important for governments to step in and ensure that there are more stringent demands. This TRIPS waiver, for me, serves as a global solution to this global problem.”
But after a year and a half of negotiations, international politics and Big Pharma’s goal of maximizing profits continue to keep plenty of production opportunities around the globe untapped.
In March, Politico reported that the EU, South Africa, India, and the US had reached a compromise, although subsequent reports said agreement was still under consideration. The compromise proposal has some key limitations. Firstly, it only addresses COVID-19 vaccines, leaving out tests and treatments, the latter of which are particularly important at this stage of the pandemic. Secondly, it only applies to patents and leaves out other critical IP like manufacturing know-how and undisclosed clinical data, which would actively enable other producers to undertake production.
As we’ve seen throughout this pandemic, the model of charity and donations that the world continues to rely on is neither sustainable nor equitable in times of global crises. The Global South needs its own COVID-19 vaccine production and supply access to prepare for new variants that may emerge. Otherwise, the cycle will begin again — rich countries will panic and hoard the best vaccines, while other countries will be forced to wait and become an opportune field in which the virus can spread and mutate. It benefits all countries, rich and poor, to empower the Global South with the technology and know-how to produce their own tools, especially when people’s lives are on the line.
Moving Forward, Collectively
Despite the emotional and physical toll of the pandemic, and the job’s low salary, Mhlongo says she’s not going to stop doing health work. She says it’s the love she has for her community that keeps her going.
“They make it hard for us — we go on long journeys to help people, but when it comes to payment, the government only pays us 3,700 rand [US $230] per month,” Mhlongo said. “Tell me, what can you do with 3,700? But even if my cooking business goes well and grows big, I won’t stop being a community health worker. We’re still going to do it because people are still there, people are still sick, people still need our services.”
 Noluthando Mhlongo rests at home for a moment before heading to work at the Phoenix Community Health Centre in Phoenix, north of Durban, on March 14, 2022.
Noluthando Mhlongo rests at home for a moment before heading to work at the Phoenix Community Health Centre in Phoenix, north of Durban, on March 14, 2022.
As the neighborhood chef and community health worker, Mhlongo is known by everyone in her area. A taxi driver once joked that she should be the mayor because everyone they passed by greeted her. In the neighborhoods that are dangerous for women and girls, there are locals who see her as part of the community and keep an eye out for her.
This idea of community is mirrored in Africa’s recent efforts to take things into its own hands.
With help from the WHO, academics, local industry, and international partners, the continent established an mRNA vaccine technology transfer hub in Cape Town, South Africa. The hub gathers and shares knowledge with the purpose of scaling up mRNA vaccine production in low- and middle-income countries.
Since pharmaceutical companies refused to voluntarily share COVID-19 mRNA vaccine knowledge so that low- and middle-income countries could start producing vaccines on an accelerated timeline, the hub decided to gather the minds and resources needed to crack the code to Moderna’s mRNA vaccine using publicly available data.
In February, Afrigen Biologics and Vaccines, a pharmaceutical startup that serves as the hub’s headquarters, accomplished this mind-bending task and made its own version of the shot, which could be tested in humans before the end of 2022. The vaccine candidate, one that the hub aims to improve on from the original, would be the first mRNA vaccine designed and developed on the African continent.
The hub has already shared its newfound mRNA technology with companies, or hub “spokes,” in 15 countries across Latin America, Africa, and Southeast Asia. These countries are also being trained on how to use the technology.
“That narrative that people have the right to prioritize their own populations — it doesn’t make sense,” policy analyst Flowers-Wanjie said. “There is a real commitment to individualism in the Global North, but across the Global South, people continuously show that it is actually community power, community support, communities coming together, that gets people through these crises.”
Afrigen is now tasked with taking its vaccine candidate through the clinical trial phase and figuring out how to replicate it on an industrial scale. This is where, again, the sharing of knowledge could change the entire story. If the hub had access to the data needed to avoid duplicating clinical trials, and the know-how needed to scale up manufacturing, it could reduce the time it would take to have an approved vaccine ready for mass production from three years down to one. From there, it hopes to go beyond COVID-19 and apply its learnings and technology towards tackling other diseases.
This collective approach should serve as an inspiration to the global community on the path to ending vaccine inequity and, more generally, health inequity.
“Re-engineering the system would take a lot,” Sehoma said. “The system has always been like this — it’s always served higher-income countries. So, changing that means changing history in its entirety. It’s much greater than COVID.”
Disclosure: This piece was made possible with funding from the Bill and Melinda Gates Foundation. It was produced with full editorial independence.