In March, as Uganda closed its borders following the first positive case of the coronavirus in the country, Rebecca Rachel Apolot realized she would not be able to return home.
“I cried everyday,” she told Global Citizen. “I don’t know how I got through.”
In January, the epidemiologist had left her family and home in Uganda to travel to Bangladesh, where she would spend two months helping the World Health Organization (WHO) control the spread of an acute water diarrhea outbreak in Cox’s Bazar.
Just as Apolot’s contract wrapped up and she expected to return home, she was stuck.
“The fact that I wasn’t close to my son to make sure he was safe was my main concern,” Apolot said, referencing her 13-month-old son Josiah. “When I was thinking about my son and being stuck here [in Bangladesh], I felt there are more vulnerable people here, more vulnerable babies here.”
As Apolot kept in touch with family through daily video calls, she turned her attention to preventing the spread of COVID-19 in the refugee camp.
 WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (right) speaks with a doctor at a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp.
WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (right) speaks with a doctor at a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp.
WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (right) speaks with a doctor at a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp.
Countries around the world began to report cases of the virus. Apolot, an infection prevention and control consultant, knew it was a matter of time before it would reach the refugee settlement.
“We said if someone is unwell, keep a distance, but it’s not very possible in the camp because one little shelter is shared by the whole family — you can’t keep a [physical] distance,” she explained.
Due to targeted violence of the Rohingya people, an ethnic minority in Myanmar, a mass exodus has made Cox’s Bazar, a town on the southeast coast of Bangladesh, the world’s biggest refugee settlement, hosting more than 860,000 refugees.
 (L) Overhead view of the world's largest refugee camp in Cox's Bazar, Bangladesh, July 2020. (R) Rohingya mothers arrive with their sick children in the health care facilities for treatment in Cox's Bazar, July 2020.
(L) Overhead view of the world's largest refugee camp in Cox's Bazar, Bangladesh, July 2020. (R) Rohingya mothers arrive with their sick children in the health care facilities for treatment in Cox's Bazar, July 2020.
(L) Overhead view of the world's largest refugee camp in Cox's Bazar, Bangladesh, July 2020. (R) Rohingya mothers arrive with their sick children in the health care facilities for treatment in Cox's Bazar, July 2020.
In addition to high congestion in the camps, the lack of ventilation in homes, and the communal use of latrines and water points were particularly concerning for health experts, who, according to Apolot, predicted that the camps would see 1,000 COVID-19 infections per day, which would have disastrous effects.
“We were thinking it would spread like wildfire,” Apolot said.
To prevent this, the WHO set up checkpoints outside the refugee settlement where people arriving to the camp would have their temperatures taken and would be screened for symptoms.
In April, the WHO and global partners launched the Access to COVID-19 Tool (ACT) Accelerator to ramp up efforts against the virus by quickly developing tests, treatments, and vaccines, as well as working to strengthen the world’s most fragile health systems, like those in Cox’s Bazar.
Apolot and the WHO team worked with the government of Bangladesh and humanitarian organizations to coordinate their outbreak response. The camp, which has 96 health posts and 36 primary health care centers, needed additional facilities to treat patients with coronavirus.
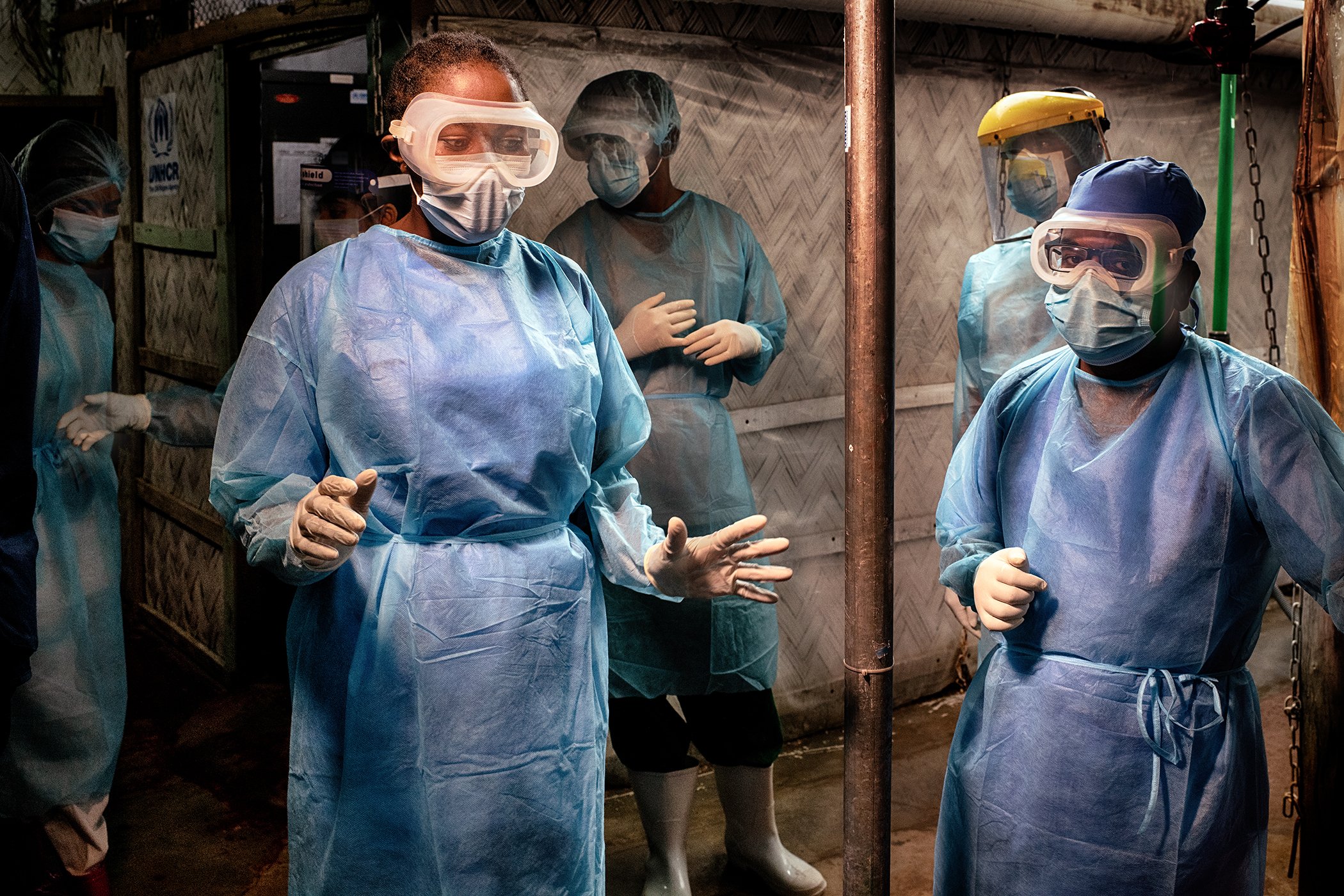 WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (left) is pictured in a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp.
WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (left) is pictured in a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp.
WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (left) is pictured in a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp.
Within months, 15 new facilities were designed and constructed according to WHO standards.
“We were ready, we had the beds and everything. By the time we had our first case, we had our personal protective equipment, we had our oxygen — everything was set.”
This was far from the case in Sierra Leone, where Apolot responded to the Ebola outbreak in 2014 and 2015.
“The world knew this [COVID-19] was coming. In Sierra Leone, where we wanted to have treatment centers, people were already dying in homes — we didn’t have quarantine centers,” she said.
Although Bangladesh reported its first COVID-19 cases in March, it wasn’t until May that the first case was reported in Cox’s Bazar.
As of Dec. 21, there were as a result of the virus in Bangladesh.
Among the Rohingya refugees in Cox’s Bazar, as of Dec. 8, there were fewer than 400 cases of COVID-19 and 10 deaths. Among the host community, there have been more than 5,000 cases and 73 deaths, Apolot told Global Citizen.
“The numbers are much, much, much lower [than projections], they're not even 10% of what was projected per day,” she said about Cox’s Bazar. “We prepared quite a lot of beds and we have never filled them to capacity.”
 Nurresha waits with her child to take a COVID-19 test in a health care facility in a Rohingya camp in Cox's Bazar, Bangladesh, July 2020.
Nurresha waits with her child to take a COVID-19 test in a health care facility in a Rohingya camp in Cox's Bazar, Bangladesh, July 2020.
Nurresha waits with her child to take a COVID-19 test in a health care facility in a Rohingya camp in Cox's Bazar, Bangladesh, July 2020.
Apolot found major gaps when assessing disease prevention and infection control in the camp. She used WHO materials to create guidelines and checklists for health workers in the camp to improve health, sanitation, and hygiene standards, such as the sterilization of equipment. Alongside a team, Apolot trained 43 health care workers — who then trained more than 2,600 others throughout the camp.
She also helped develop videos for humanitarian workers and refugees on topics such as hand-washing and physical distancing.
On a typical day, Apolot travels to various health facilities and patient wards in the camp to assess their operations, and investigates any cases of COVID-19 infections among health care workers.
“The [coronavirus response] coordination here is super, and the truth is that there is money for the response,” she said.
When Uganda opened its borders in October, Apolot went home to see her family, but decided that she would return to Cox’s Bazar, to continue her work.
“The first time [I left Josiah], I cried the whole way from Uganda to Doha,” Apolot said. “This time, I only cried when I was leaving home, giving him a hug, and grandma said, ‘You have to leave mommy. You have to let her go.’”
Apolot, who chats with her family every day — and tells Josiah a bedtime story every night — said she is thankful for technology, and for colleagues in Cox’s Bazar who can all relate to being far from their families, but whose unwavering commitment to responding to COVID-19 in the refugee settlement is admirable.
“I feel this is the best thing I can do for humanity,” she said. “This is the best thing I can offer.”
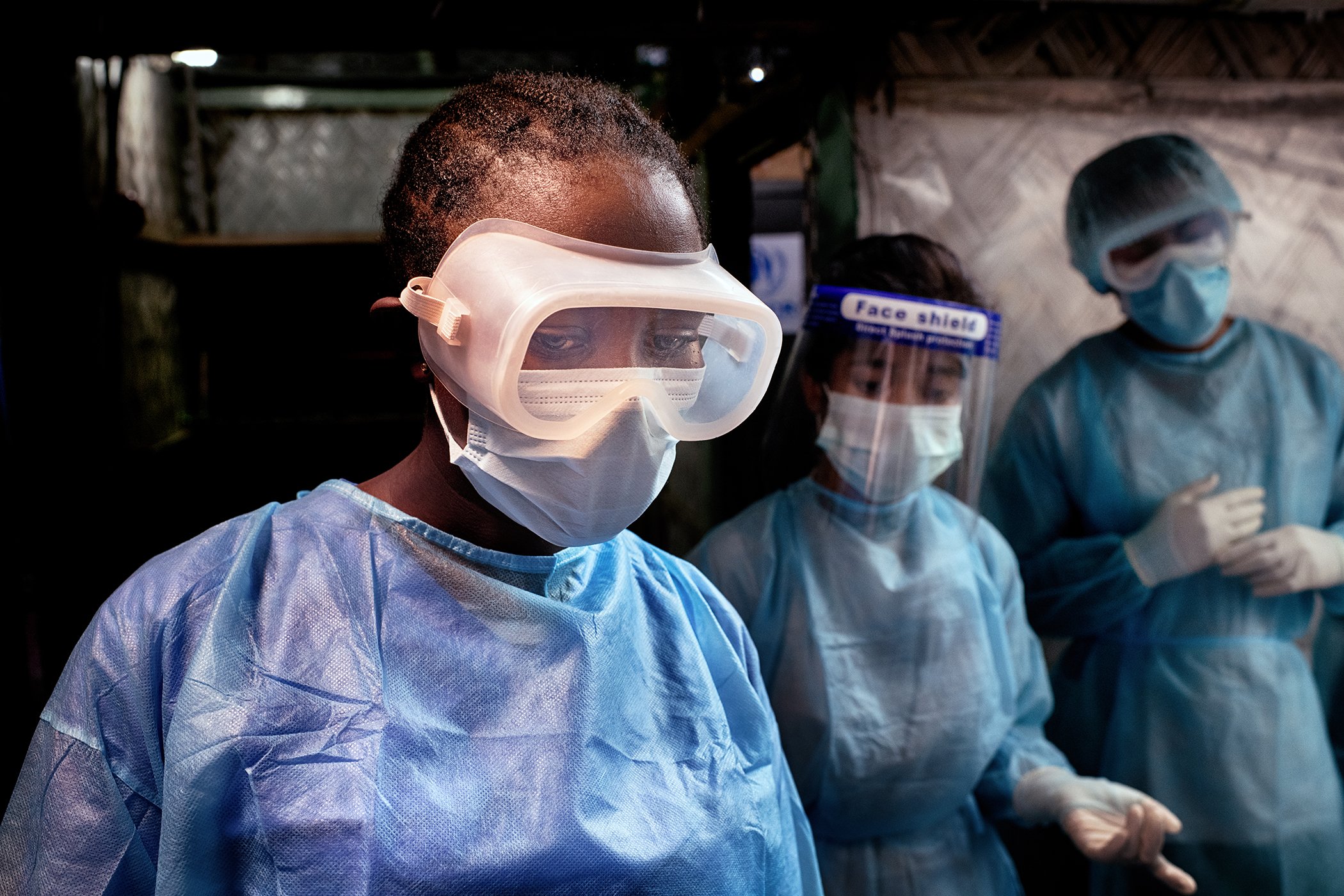 WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (left) is pictured in a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp. “I feel this is the best thing I can do for humanity,” she said.
WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (left) is pictured in a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp. “I feel this is the best thing I can do for humanity,” she said.
WHO Infection Prevention and Control Specialist Rebecca Rachel Apolot (left) is pictured in a Severe Acute Respiratory Infection Isolation and Treatment Center (SARI ITC) in a Rohingya camp. “I feel this is the best thing I can do for humanity,” she said. “This is the best thing I can offer.”
Following the A-Team is a content series that profiles the women working on the ground to combat COVID-19 via the ACT-Accelerator.
Launched in April by seven global partners, the ACT-Accelerator is a unique coalition aimed at accelerating global efforts against the COVID-19 pandemic. Its members are working together to develop tests, treatments, and vaccines as quickly as possible, while also strengthening the world’s most fragile health systems.
The organization desperately needs financial support from governments around the world. You can join us in calling on world leaders to fund the ACT-Accelerator by taking action here.
Disclosure: This series was made possible with funding from the Bill and Melinda Gates Foundation. Each piece was produced with full editorial independence.