Amina Ismail is a surveillance officer for the World Health Organization (WHO) working to trace and identify polio in Kenya. She spends her days tracking the virus in some of the most remote areas of the country, because she knows that to eradicate polio, it is critical to find every last virus as well as reaching every last child with vaccines.

Disease detectives like Amina know from personal experience that the data at the heart of the surveillance system is not just for number crunching and spreadsheets. It’s the difference between whether or not a child is reached with life-saving vaccines; it means healthcare centres equipped with the knowledge they need to give families the services they need; and it means countries carrying out well planned immunization activities. It makes the difference between stopping a disease like polio and allowing it to continue to circulate unnoticed.
The essential role of surveillance for polio eradication
[The] wild poliovirus is present in fewer areas of the world than it has ever been in human history. We know this because the polio programme’s surveillance system goes to great lengths so that no case slips through the net unnoticed.
Amina is one of a team of seven WHO surveillance officers in Kenya who work alongside Ministry of Health and other partner organizations of the Global Polio Eradication Initiative (GPEI).
Reporting every case
Amina visits healthcare centres, schools, traditional healers, community leaders, parents and many others in her work to ensure that the surveillance system in Kenya is alert to any sign of polio. This week, she travels along a dirt track to Ciakagira Health Centre where Amina meets with Emily, the nurse in charge. Amina asks Emily what symptoms would alert her to the possible presence of polio, and Emily describes acute flaccid paralysis- floppy, paralysed arms and legs with no obvious cause. Healthcare workers having this knowledge at their fingertips is what enables the surveillance system to find each child who may have polio, to test them, and then to trigger an outbreak response if the sample comes back positive.

Every week, Emily sends a report of the number of cases of acute flaccid paralysis from Ciakagira to the data team at county level, which feeds up into national and global planning for polio eradication. “I am here to support you, not to root for mistakes- a new pair of eyes see the cobwebs easier than the home owner,” Amina reassures her as she goes through the clinics’ case registers to check the quality of the data.
Data speaks
This data is not just for use at global and national level for planning. Amina explains that every time the data shows that a child has been infected with a vaccine preventable disease, the doctors and nurses need to go back and question the whole system: checking whether children are missing doses of vaccines, ensuring that the cold chains are storing the vaccines safely, exploring how communities are being engaged, all to find out why the child was left unprotected.
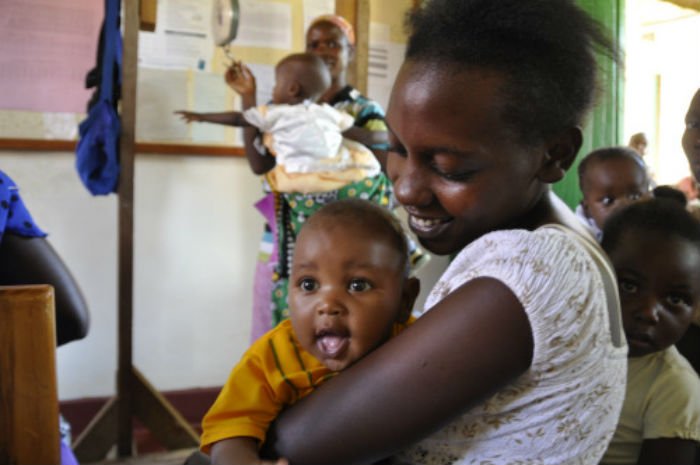
Beyond polio
As the prospect of a polio-free world draws ever closer, the role of the polio surveillance system is increasing in importance. Not only does it provide the partners of the GPEI with the data they need to be sure that the virus is gone for good; but the strong global network established for polio is also helping to trace and stop other diseases, such as measles and tetanus.
“We are getting to the endgame of polio- it is time to go beyond health systems and into the community,” explains Amina.
The polio eradication programme has an incredible legacy for children everywhere. The knowledge, skills and staff of the programme have much to offer other programmes and communities.
Legacy in action
The work done by Amina and her colleagues is a perfect example of the polio legacy in action. As Amina asks healthcare workers, traditional healers and teachers about polio, she also tests their knowledge of measles and neonatal tetanus, and ensures that these cases are also being reported. At each clinic, she goes through routine immunization data, ensuring that no children are being missed for follow up doses without which their protection would be incomplete.

Being certain that a virus really is gone from each country, and later from the entire planet, is the biggest question asked by any eradication programme. The GPEI [celebrates] the disease detectives who make it possible to find the answer.
It is people like Amina who form the lifeblood of polio surveillance, building knowledge at local level, checking that each detail is fed correctly into the system, and strengthening that system so it can inform how we keep children safe.
Polio eradication will be one of the greatest achievements of the age. But equally, the lessons, resources and infrastructure of the programme will continue to help children for generations to come.
This article was written by Leilia Dore, World Health Organization, in support of Gavi, the Vaccine Alliance.